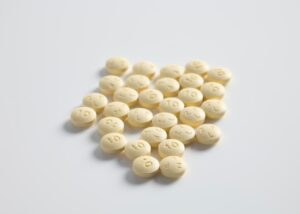
Are drug dealers promoting the new super-potent opioids, metonitazene and para-fluorofentanyl?
Heroin users rarely know what they are getting anymore. What do their dealers tell them?
Has a drug dealer ever told a customer that they are now selling metonitazene? What about para-fluorofentanyl, also known as “China-white?”
Some drug dealers take the completely dishonest route, telling their customers that they are only selling pure heroin. I have spoken to people who swear that they have an honest and trustworthy heroin dealer.
They have the one dealer who only sells the pure stuff, real heroin. They know how to avoid fentanyl-like contaminants.
Yet, when they come into the office and get a urine drug screen, we see the results come up with fentanyl and no heroin. What about the honest dealer? Were they also tricked by their supplier?
The truth is that no one knows what is being sold on the streets as heroin anymore.
The only thing that we can be fairly certain of is that very little, if any, of it contains any heroin whatsoever. So, how did metonitazene, an opioid drug from the 1950s that never gained approval for medical treatment, resurface? And, what about para-fluorofentanyl, a synthetic opioid from the 1960s?
We do know that designer opioids are imported from China. Some people believe that clandestine opioid labs in China are always working to skirt local laws by changing the opioid molecules to something that is not yet illegal.
In the US, there are analog drug laws that can effectively outlaw a new exotic opioid variation that a lab might produce, before law enforcement has the chance to study and identify it. In China, there are no such laws.
American federal officials work quickly to outlaw new opioids as they identify them in the street supply that was once known as “heroin.” For example, there are seven synthetic benzimidazole-opioid substances that were recently announced as being added to the list of schedule I narcotics, along with heroin.
These include metonitazene, and also metodesnitazene, butonitazene, etonitazene, protonitazene, etodesnitazene, flunitazene, and n-pyrrolidino. How do doctors keep up, with testing for all of these opioid substances?
Synthetic opioids are becoming more and more prevalent.
Unfortunately, each of these drugs would have to be tested for separately, and addiction treatment centers are not prepared for that. Many people believe that there is a drug test that screens for all opioids.
This is simply not true. There is a test for both morphine and heroin, which are closely related, but not for all other opioids. For example, if a person has been taking only oxycodone, and a doctor only screens for morphine and heroin, the test will come up negative.
In fact, the only way that researchers know that these drugs are showing up on the streets is when they perform advanced toxicology studies on the substances that they recover. In many cases, these studies are not done, so doctors and rehabs must guess at what opioids their patients were taking.
Unfortunately, exotic, unidentified street opioids may have unique properties that interfere with drug treatment. For example, medication assisted treatment with buprenorphine or with naltrexone can be complicated by these synthetic opioid analogs.
The problem is that we are calling everything masquerading as heroin, fentanyl. The fact is that much of this “fentanyl” does not share basic properties with pharmaceutical, legal fentanyl.
For example, street fentanyl can linger in the drug user’s system for days, making it difficult to start Suboxone treatment. Doctors must learn new techniques for starting Suboxone therapy, such as the Bernese Method, or microdosing Suboxone.
What is the solution to reducing overdose deaths due to this wide variety of toxic, potent opioids sold as heroin?
The answer to preventing deaths due to a toxic drug supply is to make the drug supply safer. This is a form of harm reduction.
What happens when a doctor prescribes fentanyl patches to a patient with cancer pain? Imagine if the doctor said, “let’s cross our fingers and hope that this stuff is not too strong for you to handle.”
That would never happen, because the doctor, and pharmacist, know precisely the strength and pharmacological properties of the drug being prescribed. There is no question of what to do if the fentanyl patch turns out to be 10x or 100x the expected strength.
In fact, in British Columbia, Canada, some doctors are prescribing fentanyl patches to people addicted to street opioids. The purpose of this is to reduce overdoses caused by street opioids of unknown potency.
What is the precontemplation stage of addiction recovery?
There are multiple stages of readiness to overcome addiction. The first stage is known as “precontemplation.”
This means that the person is not ready at all to consider stopping their drug use. It does not mean at all that they are hopeless and that they will never be ready. It simply means that they are not ready for now.
Addiction experts, family members, loved ones, and law enforcement personnel have struggled with the issue of precontemplation, even without fully understanding it. They have tried many ways to force people stuck in active addiction to be ready to get help.
Experience has demonstrated that forcing someone out of the precontemplation stage does not always work. Attempting to force a person out of their addiction can be frustrating.
While options to forcing someone into treatment, such as the Florida Marchman Act, can be lifesaving, and give a person time and space to move beyond precontemplation, often this is not practical for many people addicted to dangerous street drugs. Another alternative is to provide harm reduction efforts to keep people alive and safe, for when they are finally ready to ask for help.
British Columbia government officials have found that by allowing for the drug supply to be made safer, with prescription heroin, Dilaudid dispensing machines, and fentanyl patch prescriptions, fewer people are dying from opioid overdoses. They also have supervised consumption centers, where people can use heroin-like substances under supervision, with safe paraphernalia.
Why has the war on drugs been unsuccessful?
The fact that the war on drugs has failed so far does not mean that we should give up on the fight. What it does mean is that we must change our tactics.
Locking people up for drug use has not been an effective way of slowing down drug addiction and overdoses. Decriminalizing drug use and providing harm reduction strategies has made a positive difference.
By reducing the stigma associated with drug addiction and making effective, proven addiction treatments more readily available, we can help more people to overcome addiction. While stopping the influx of deadly opioids from China and Mexico is important, we must also improve drug education and, especially addiction treatment.
While metonitazene, para-fluorofentanyl present serious dangers to drug users, along with many other opioids and opioid-like substances, we do have the tools to help people quit these drugs. Medication assisted treatment for opioid addiction works, regardless of the opioid in question.
By streamlining and improving medication-assisted treatment protocols, and making these treatments available to everyone who needs them, we can start to reduce the overdose numbers significantly. Now is the time to take the opioid epidemic as seriously as any other dangerous epidemic and take the necessary action to protect people from the dangers of toxic street opioids.